We all know vitamins are good for us, but did you know some of them are frequently consumed in inappropriate amounts? Vitamins such as Vitamin D, Vitamin A, Vitamin B6 (pyridoxine), and Vitamin B3 (niacin) are among the most commonly misdosed nutrients.
Why does this happen? These vitamins are widely available, commonly recommended, and often perceived as completely safe even at higher doses. As a result, many individuals take additional supplements in hopes of improving energy levels, boosting immunity, or enhancing skin health, without realizing that excessive intake can lead to adverse effects.
Before choosing your supplements, it’s worth reading our blog: Which Vitamins Are Commonly Non-Vegetarian?
An important challenge is that symptoms of vitamin excess (hypervitaminosis) are often subtle and develop gradually, making them easy to overlook. Depending on the vitamin, excessive intake may lead to toxicity affecting the liver, nervous system, or metabolic balance. So, it’s important to know which vitamins are most often misdosed and why. Let us read on to know more.

What Are the Most Commonly Misdosed Vitamins?
Not all vitamins are misdosed equally; some are far more likely to be taken in the wrong amounts, either too much or too little. A key concern is that many individuals may not realize they are exceeding recommended limits, especially when combining dietary intake with supplements.
Let’s take a closer look at some of the most commonly misdosed vitamins:
- Vitamin D3: Widely used for bone health and immune support, Vitamin D3 is one of the most commonly over-supplemented nutrients. Excess intake can lead to hypercalcemia (elevated blood calcium levels), which may cause nausea, vomiting, kidney dysfunction, and, in severe cases, calcification of soft tissues.
Concerned about kidney health and supplements? Explore our blog: Your Kidney Guardians – What to Eat, What to Avoid, and Why It Matters.
- Vitamin A: Commonly found in supplements for vision and skin health, Vitamin A is fat-soluble and accumulates in the body. Chronic excessive intake can result in toxicity, leading to headaches, liver damage, dizziness, and blurred vision.
- Vitamin B6: (Pyridoxine): Important for nerve function and metabolism, Vitamin B6 is often used to support mood and energy. However, prolonged intake of high doses can cause peripheral neuropathy, characterized by tingling, numbness, or nerve damage.
- Vitamin B3 (Niacin): Used in certain cases to help manage cholesterol levels, niacin can cause flushing (warmth and redness of the skin) even at moderate doses. Higher doses may lead to liver toxicity, gastrointestinal disturbances, and impaired glucose tolerance.
- Vitamin E: Known for its antioxidant properties, Vitamin E is commonly taken for skin and heart health. Excessive intake may increase the risk of bleeding, particularly in individuals on anticoagulant therapy (blood thinners), and has been associated in some studies with an increased risk of hemorrhagic stroke.
These vitamins are essential, but they’re also the ones that are easiest to misdose. The key takeaway? More isn’t always better, especially when it comes to fat-soluble vitamins that stay in your system longer.
Curious about antioxidant-rich vitamins? Explore our blog: The Antioxidant Shield: Your Body’s First Line of Defense Against Disease.

Read more: https://www.ncbi.nlm.nih.gov/books/NBK538510/
Water-Soluble vs. Fat-Soluble: Why It Matters
Vitamins are broadly classified into two categories: water-soluble and fat-soluble, and this distinction plays a crucial role in how the body absorbs, utilizes, and eliminates them.
Water-soluble vitamins like vitamin C and the B-complex group dissolve in water and are not extensively stored in the body, which means they leave your body through urine. So even if you take a bit more, your body usually flushes it out. However, this also means they need to be consumed regularly to maintain adequate levels.
In contrast, fat-soluble vitamins like A, D, E, and K are absorbed along with dietary fats and stored in the liver and adipose (fat) tissues. Because they are retained in the body, excessive intake over time can lead to accumulation and increase the risk of toxicity or adverse health effects. That’s why fat-soluble ones need extra care.
Why Water-Soluble Vitamins Are Safer (But Not Risk-Free)
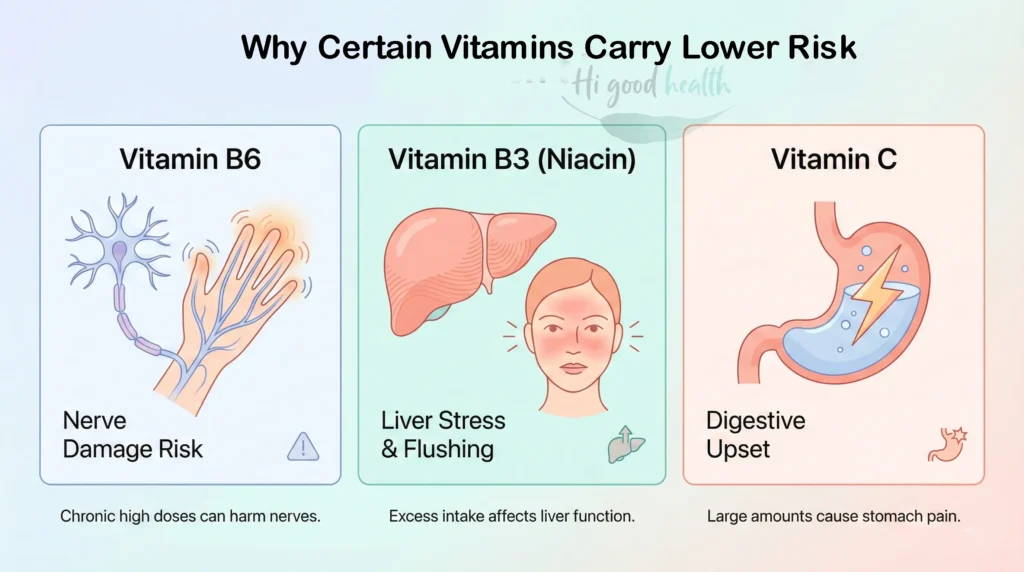
Although the water-soluble vitamins are excreted through urine, this doesn’t mean that they are completely risk-free. For instance, high doses of vitamin B6 (pyridoxine) over prolonged periods have been linked to sensory neuropathy, causing symptoms such as numbness, tingling, and difficulty walking.
Similarly, niacin (vitamin B3) at doses above 1–3 grams per day can lead to liver toxicity and severe flushing, sometimes accompanied by nausea and abdominal pain.
Even vitamin C, often seen as harmless, can cause gastrointestinal disturbances like diarrhoea, cramps, and nausea when taken in doses over 2,000 mg per day. In rare cases, extremely high doses may trigger migraines.
So, while the body’s ability to flush out excess water-soluble vitamins generally protects you, consistently exceeding recommended intakes can lead to serious health issues. It’s important to follow dosing guidelines even for these “safer” vitamins.
Fat-Soluble Vitamins: Small Overdose, Big Trouble
Unlike water-soluble vitamins that are readily excreted, even relatively small excesses of fat-soluble vitamins can lead to significant health complications due to their ability to accumulate in the body over time.
Vitamin A overdose can lead to symptoms like headaches, nausea, dizziness, and in severe cases, liver damage, bone pain, and increased pressure inside the skull. Too much Vitamin A during pregnancy causes birth defects (>10,000 IU/day during pregnancy is associated with teratogenic effects).
Overconsumption of Vitamin D can lead to hypercalcemia (elevated blood calcium levels), which may cause nausea, vomiting, weakness, kidney dysfunction, and, in severe cases, cardiac arrhythmias and soft tissue calcification.
Vitamin E in excess can interfere with the normal blood clotting mechanism, raising the chance of bleeding problems and stroke, especially if you’re on blood thinners.
Because these vitamins are stored in the liver and fatty tissues, chronic intake above recommended levels, even if only slightly excessive, can result in gradual accumulation and toxicity. Therefore, careful attention to dosage is essential when using supplements.
**If you experience symptoms of vitamin overdose, such as severe nausea, confusion, irregular heartbeat, or other concerning symptoms, seek immediate medical attention or contact the U.S. Poison Control hotline at 1-800-222-1222 (available 24/7).
Read More: NIH / NCBI Vitamin D toxicity overview
Check out the Verified Normal Blood Test Reference Ranges:
| Vitamin | Typical Reference Range | Units | Notes |
| Vitamin D3 (25(OH)D) | 20 – 50 (sometimes 30 – 100) | ng/mL | Levels <20 ng/mL usually indicate deficiency; some labs set sufficiency at >30 ng/mL. |
| Vitamin A | 20 – 60 | mcg/dL | Serum retinol levels; some labs report in μmol/L (0.7–2.2 μmol/L). |
| Vitamin B6 | 5 – 50 | ng/mL | Measured as pyridoxal 5′-phosphate (PLP), the active form of B6. |
| Vitamin E | 5.5 – 17 | mg/L | Typically measured as alpha-tocopherol. |
| Vitamin B12 | 200 – 900 | pg/mL | Levels <200 pg/mL generally suggest a deficiency. |
Important Notes:
- Vitamin D: Serum 25-hydroxyvitamin D [25(OH)D] is the standard test. Some labs consider >30 ng/mL as optimal; below 20 ng/mL is usually deficient.
- Vitamin A: Measured as serum retinol Units can vary (mcg/dL or μmol/L), so be sure to match your lab’s units.
- Vitamin B6: The active form, pyridoxal 5′-phosphate (PLP), is typically tested.
- Vitamin E: Labs measure alpha-tocopherol; values can vary by lab and population.
- Vitamin B12: Deficiency is generally below 200 pg/mL. Additional markers (such as methylmalonic acid or homocysteine) may be used for confirmation.
How to Know How Much Vitamin You Really Need
Not everyone needs the same amount of vitamins. Your ideal dose depends on your age, diet, medical conditions, and whether a true deficiency is present.
Relying on supplements based solely on general recommendations, product labels, or trends can be misleading and, in some cases, harmful. Excess intake, especially without a confirmed deficiency, may increase the risk of adverse effects or toxicity. The safest way to find out what your body needs is by getting tested. Here’s a simple guide to which blood tests help identify specific vitamins and mineral deficiencies.
Looking for the right supplement guidance as you age? Explore our blog:
| Nutrient | Blood Test | Deficiency Signs |
| Vitamin D | 25(OH)D (25-hydroxyvitamin D) | Weak bones, fatigue, and low immunity |
| Vitamin B12 | Serum B12 | Tingling hands/feet, memory issues |
| Iron | Ferritin, Iron, TIBC | Fatigue, pale skin, short breath |
| Folate (B9) | Serum folate | Mouth sores, poor concentration |
| Magnesium | Serum magnesium | Muscle cramps, irregular heartbeat |
| Calcium | Serum calcium | Muscle spasms, brittle nails |
| Zinc | Plasma zinc | Hair loss, slow wound healing |
| Omega-3 | Omega-3 Index or RBC EPA/DHA | Dry skin, brain fog, joint pain |
| Iodine | Urinary iodine concentration | Thyroid issues, weight gain |
Read more: https://www.betterhealth.vic.gov.au/health/healthyliving/vitamin-and-mineral-supplements
How to Avoid Vitamin Misdosing in Daily Life
Vitamin overdosing is more common than people think, and it often happens unintentionally. To stay safe and get the full benefit of your supplements, here are a few medically sound tips:
1 Consult a healthcare professional
Before starting any supplement, speak to a healthcare professional. Your doctor may recommend blood tests to assess actual needs and avoid unnecessary intake.
Wondering which diagnostic tests are truly necessary? Explore our blog: Are Frequent Blood & Other Diagnostic Tests Really Necessary?
2. Avoid high-dose supplements Unless Prescribed
More is not always better. High doses of fat-soluble vitamins (A, D, E, K) can build up in the body and cause toxicity.
3. Track Your Supplement Intake
Keep a log of all vitamins, multivitamins, minerals, and herbal products you take. Overlapping ingredients can quietly lead to overdosing.
Curious about what your multivitamin might be missing? Read our blog: 60+ Essential Minerals That Protected Our Ancestors but Are Missing from Your Multivitamin.
4. Check for Fortified Foods
Many packaged foods, such as cereals, juices, and snacks, are fortified with extra vitamins. When combined with supplements, this may result in intake exceeding recommended limits.
5. Read Labels Carefully
Watch for the % Daily Value (%DV). Anything over 100% should raise a red flag unless medically required.
6. Reassess Regularly
Nutritional requirements change with age, health conditions, dietary patterns, and lifestyle. Periodic reassessment helps ensure that supplementation remains appropriate and necessary.
Key Takeaways
- Your best approach is a personalized one.
- Do not rely on general recommendations or online trends.
- Testing, tracking, and tailoring your supplement use is key to safe and effective nutrition.
FAQ
1. Can taking vitamins actually be harmful?
Yes. While vitamins are essential, too much of a good thing can actually be harmful. High doses, especially of fat-soluble vitamins, can accumulate in the body and cause toxicity, organ damage, or long-term health issues.
2. Which vitamins are most dangerous to overdose on?
Fat-soluble vitamins like A, D, E, and K are the riskiest because they are stored in fat tissues. However, water-soluble vitamins like B6 and Niacin can also cause nerve or liver damage if taken in high doses.
3. What are the common symptoms of vitamin overdose?
Symptoms often “creep in slowly” and can include nausea, headaches, weakness, and digestive upset. High doses of Vitamin B6 specifically can lead to a tingling sensation or numbness in the hands and feet.
4. Is it safe to take Vitamin C or B vitamins in large amounts?
Not necessarily. While the body flushes excess water-soluble vitamins, high doses are not risk-free. Vitamin C over 2,000 mg can cause cramps and nausea, while long-term high B6 intake is linked to nerve damage.
5. How do I know if I actually need supplements?
“The safest way to find out what your body needs is by getting tested” rather than guessing. Blood tests like 25(OH)D for Vitamin D can confirm actual deficiencies, preventing you from taking “random supplements” unnecessarily.
6. Can I take supplements if I eat fortified foods?
Be cautious. Many cereals, juices, and snacks are fortified with extra vitamins. If you combine these with supplements, you might unknowingly exceed safe limits, so it is vital to read labels carefully.
7. Should I take a supplement every day?
Not everyone needs the same amount. Your ideal dose depends on your “age, diet, medical conditions,” and deficiency status. Consult a doctor to tailor your intake rather than relying on general trends or “random supplements”.
8. What should I do if I suspect a vitamin overdose?
If you experience severe symptoms like confusion, irregular heartbeat, severe nausea, or other concerning signs after taking vitamins, seek immediate medical attention. You can also contact the U.S. Poison Control hotline at 1-800-222-1222, which is available 24/7 and staffed by medical experts.
All reference links valid and accessible on 29 April 2026
- Hathcock, J. N., Shao, A., Vieth, R., & Heaney, R. (2007). Risk assessment for vitamin D. The American Journal of Clinical Nutrition, 85(1), 6–18.
- Marcinowska-Suchowierska, E., Kupisz-Urbańska, M., Łukaszkiewicz, J., Płudowski, P., & Jones, G. (2018). Vitamin D toxicity–A clinical perspective. Nutrients, 10(3), 1–14.
- Penniston, K. L., & Tanumihardjo, S. A. (2006). The acute and chronic toxic effects of vitamin A. The American Journal of Clinical Nutrition, 83(2), 191–201.
- Institute of Medicine (US) Panel on Micronutrients. (2000). Dietary Reference Intakes for Vitamin A, Vitamin K, Arsenic, Boron, Chromium, Copper, Iodine, Iron, Manganese, Molybdenum, Nickel, Silicon, Vanadium, and Zinc. National Academies Press.
- Institute of Medicine (US) Panel on Calcium and Vitamin D. (2011). Dietary Reference Intakes for Calcium and Vitamin D. National Academies Press.
