The hidden epidemic that’s costing families thousands while destroying health
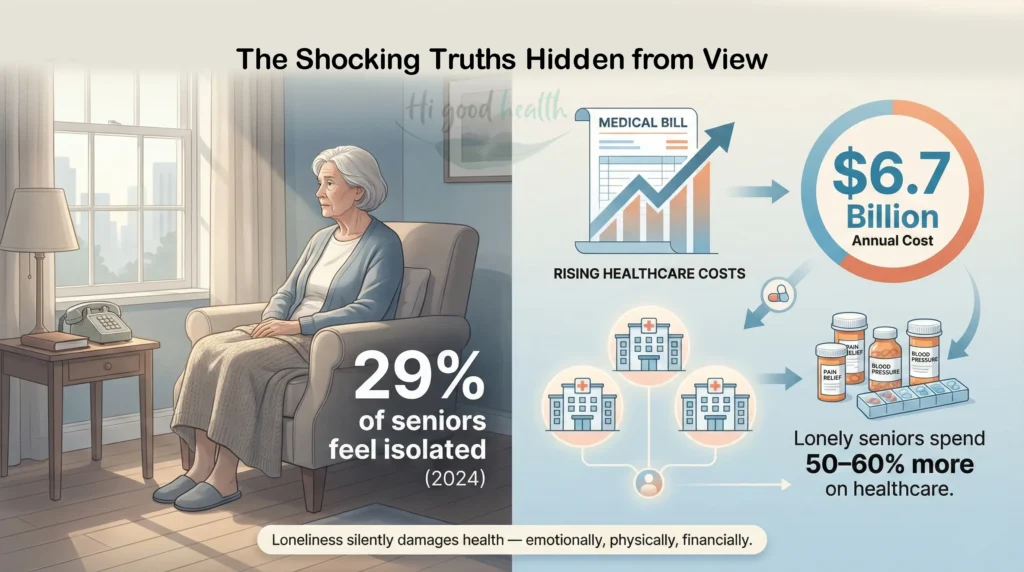
The Shocking Reality Behind Closed Doors
Sarah, 72, visits her doctor almost every month with new complaints—headaches, joint pain, sleepless nights. Her medical bills exceed $8,000 yearly. Her daughter assumes it’s normal aging.
But It’s not.
Sarah hasn’t had a meaningful conversation with anyone in weeks.
A SILENT EPIDEMIC WITH A FINANCIAL TOLL
Recent data shows 29% of older adults feel isolated some of the time or often in 2024, but the real crisis isn’t just emotional—it’s financial. Lonely seniors generate healthcare costs significantly higher than connected peers, creating a $6.7 billion annual burden on families and Medicare according to analysis from AARP and the Health and Retirement Study.
U.S. Surgeon General Dr. Vivek Murthy warns that “the degree to which our life is shortened is similar for loneliness as it is for smoking 15 cigarettes a day.” Yet unlike smoking, loneliness remains largely unrecognized and untreated.
At higoodhealth.com, we believe in sharing credible health information that empowers families to make informed decisions. This crisis affects millions of American families—and understanding it could save both lives and money.
Why Loneliness Literally Makes Seniors Sick
The Medical Evidence
Loneliness isn’t just a feeling—it triggers measurable biological changes that damage health over time.
Inflammation Overload
Chronic loneliness triggers persistent low grade inflammation, elevating C-reactive protein and interleukin-6 levels similar to severe chronic diseases. These inflammatory markers stay elevated continuously, attacking tissues throughout the body and accelerating aging at the cellular level.
Over time, this constant inflammatory state:
- Damages tissues
- Accelerates cellular aging
- Increases vulnerability to chronic illness
Learn how your daily digital habits could be fueling silent inflammation and affecting your long-term brain and gut health. Read our guide Your Digital Life & Inflammation – Spot It, Stop It, Safeguard Your Brain & Gut & Immune System
Collapse of Body’s Defense System
Research from Dr. Carla Perissinotto’s 2012 landmark study reveals that seniors who feel lonely have a **45% greater risk of death** (adjusted HR 1.45) and **59% greater risk of physical decline**. It is worth noting that these risks were found to be independent of clinical status, depression, and social network, which emphasizes the fact that loneliness is a distinct biological risk factor.
Cardiovascular Damage
Dr. Murthy’s 2023 report on loneliness shows loneliness increases risks of cardiovascular disease, dementia, stroke, depression, and anxiety. Blood pressure remains elevated, blood vessels become stiffer, and heart attack risk increases dramatically.
Reduced Cognitive Reserve
Social connection does more than provide emotional support, it builds cognitive reserve. This is the brain’s capacity to improvise and utilize alternate neural pathways to complete tasks. Frequent social engagement functions as a “mental workout,” increasing synaptic density and strengthening these networks. Research indicates that many seniors who have a good social network maintain baseline cognitive function for years, even when physical markers of Alzheimer’s or dementia are present in the brain.
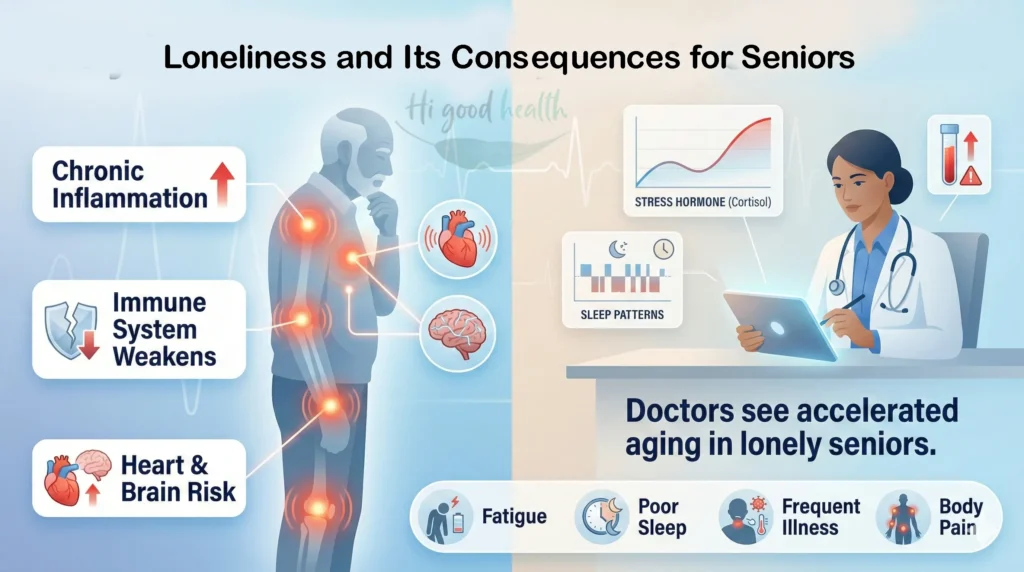
What Doctors See
In medical practice, lonely seniors present with accelerated aging—their biological age appears decades older than their chronological age. Blood work shows elevated stress hormones, disrupted sleep patterns, and inflammatory markers matching patients with serious chronic conditions.
Physical Symptoms Include:
- Persistent headaches and muscle pain
- Digestive issues and appetite changes
- Sleep disturbances and chronic fatigue
- Frequent minor infections
Discover the latest nutritional science to help seniors maintain strength and effectively prevent muscle loss. Read our Guide Senior Nutrition 2026: Prevent Muscle Loss with the Latest Science
The Hidden Financial Devastation
Healthcare Cost Explosion
The numbers tell a stark story. Medicare research shows socially isolated seniors cost Medicare approximately $1,600 more per person annually than their socially connected peers—totaling $6.7 billion across the system.
For individual families, costs accumulate across multiple areas:
Emergency Visits
Recent studies indicate lonely seniors use emergency departments significantly more often than connected peers—up to 67.8 visits per 100 beneficiaries compared to 47.9 for connected seniors.
Specialist Referrals
Increased need for pain specialists, psychiatrists, and multiple consultations. Each appointment adds copays, transportation costs, and time away from work for family caregivers.
Medication Costs
Higher prescriptions for sleep aids, pain relievers, and psychiatric medications. Monthly pharmacy bills climb as doctors try to address symptoms that stem from social disconnection.
Hospital Stays
Longer recovery times and more complications during treatment. Studies show isolated seniors experience more post-surgical complications and extended hospital stays.
Family Financial Impact
- Average Additional Costs: $3,000-5,000 annually per isolated senior in out-of-pocket expenses
- Out-of-Pocket Burden: Medicare copays and deductibles compound quickly, especially with multiple specialist visits
- Nursing Home Risk: Lonely seniors enter long-term care facilities at double the rate of connected peers, with costs exceeding $100,000 annually
Geographic Variations
Rural areas with limited social services see costs 40% higher than communities with robust senior programs. Transportation barriers, fewer healthcare options, and geographical isolation compound the problem.
Dr. Carla Perissinotto, geriatrician at UCSF, notes: “Social isolation is as predictive of early death as traditional medical risk factors, yet we rarely screen for it systematically.”
Breaking the Cycle: What Actually Works
Evidence-Based Solutions
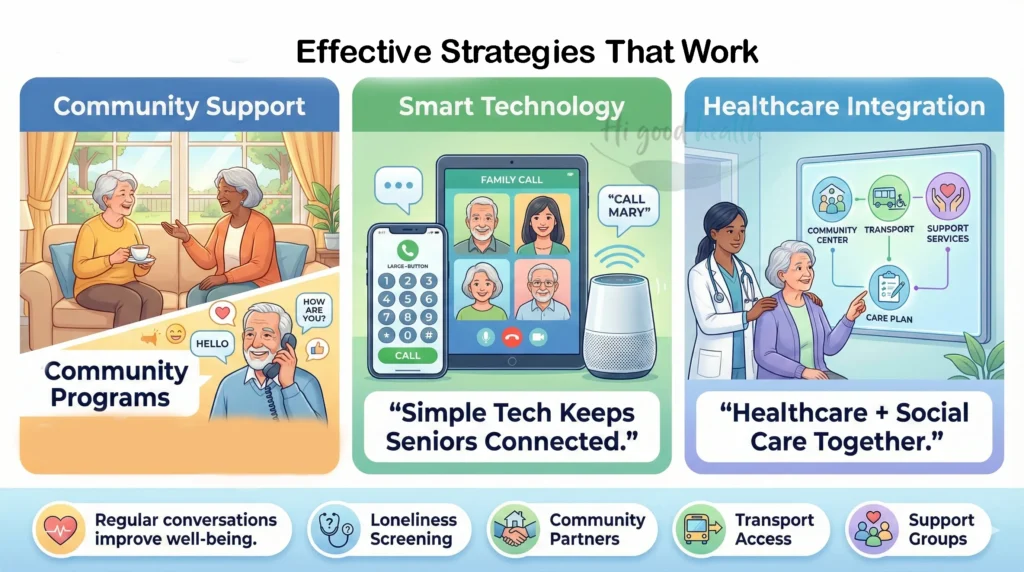
Community Programs
Programs like Oregon’s Senior Loneliness Line show measurable results, with many seniors reporting significant improvement in outlook and reduced thoughts of isolation. The program provides both friendly conversation for daily connection and crisis support when needed. Regular callers who initially expressed suicidal thoughts due to loneliness often experience dramatic positive changes as they build rapport and feel safe.
Technology That Works
When properly introduced with training, technology can bridge distance gaps:
- Large-button phones with pre-programmed contacts for easy family communication
- Tablets with simplified video interfaces for virtual visits with grandchildren
- Voice-activated emergency response systems that provide safety and peace of mind
Research shows older adults benefit most from technology training conducted by peers close to their age, delivered in group settings that provide both learning and social connection.
Intergenerational Programs
Connecting seniors with school children or young families creates mutual benefit and purpose-driven relationships. Recent systematic reviews show intergenerational interventions produce significant reductions in older adult loneliness, with some programs reporting loneliness scores dropping from 84.2% to 40% after just 6 weeks of participation.
These programs work through various activities: shared mealtimes, committee meetings involving both generations, one-on-one leisure activities, and coordinated transportation that brings age groups together naturally.
Healthcare Integration
Progressive healthcare systems now include social prescribing—formal referrals to community programs, volunteer networks, and social services as part of medical treatment. Social prescribing allows doctors to write a ‘prescription’ for non-medical activities, such as a community gardening group, a local choir, or a walking club, which are then facilitated by a ‘link worker’ who connects the senior to these resources. Evidence from Canada, the UK, and emerging U.S. programs shows this holistic approach creates stronger integration between medical care and community support systems.
Successful Models Include:
- Routine loneliness screening during medical visits using validated tools
- Partnerships between hospitals and community centers for referrals
- Transportation programs specifically for social activities
- Grief support groups integrated with healthcare systems
Find out exactly which supplements are essential for senior health and how to make plant-based eating work for your body. Read our Guide Senior Nutrition in 2026: Protein, Supplements & Plant-Based Diets
Latest Research Breakthroughs (2024-2026)
Biomarker Discovery
Recent research confirms that loneliness is not just psychological—it is measurable at the cellular level.
Telomere Shortening
Cellular aging accelerates dramatically in isolated individuals. Telomeres—the protective caps on chromosomes—shorten faster, essentially making cells age more rapidly than chronological time would predict.
Faster telomere shortening = accelerated biological aging
Cells behave as if they are older than the person’s actual age
Increased risk of age-related diseases
Gene Expression Changes
Loneliness alters how genes function:
- Upregulates inflammatory pathways
- Suppresses antiviral immune responses
This creates a dangerous dual effect:
- Chronic inflammation damages tissues
- Reduced immunity increases infection risk
Cortisol Patterns
Chronic stress hormone elevation mimics severe trauma responses. In many cases of chronic stress or loneliness, the issue is not just constant elevation but a “flattening” of the diurnal cortisol slope, where the normal morning peak is lower and the evening decline is less pronounced. This contributes to high blood pressure, weight gain, and cognitive decline.
AI and Digital Interventions
Recent AI elder care studies show promising results in battling the loneliness crisis, with voice-activated companions providing medication reminders and basic social interaction. However, research emphasizes these technologies work best as supplements to—not replacements for—human connection.
Emerging Technologies:
- Smart home monitoring for family peace of mind without intrusive surveillance
- Virtual reality social experiences designed specifically for seniors with mobility limitations
- Automated check-in systems for isolated adults that alert family members to unusual patterns
Prevention Research
New economic studies reveal that loneliness prevention programs cost approximately $1,500 per senior annually while generating healthcare savings of $3,000-4,000 per person—a clear return on investment. Research published in 2025 shows positive social return on investment ratios ranging from $2.28 to $13.72 for every dollar spent on intervention programs.
One cost-effectiveness study concluded that interventions to reduce severe loneliness in older adults are cost-effective but unlikely to be completely cost-saving, meaning society benefits economically even though some costs remain.
Warning Signs Families Must Know
Early Detection Checklist
Physical Red Flags:
- Increased medical complaints without clear causes or diagnoses
- Frequent requests for stronger pain medication when previous doses were adequate
- Changes in appetite or sleep patterns that can’t be explained medically
- Reluctance to end medical appointments—lingering in the office for conversation
Behavioral Changes:
- Avoiding previously enjoyed activities like church, clubs, or hobbies
- Declining personal hygiene or home maintenance despite physical ability
- Increased alcohol consumption as a coping mechanism
- Personality changes or increased anxiety in social situations
Communication Patterns:
- Calling family members more frequently with minor concerns
- Expressing feelings of being a burden to family
- Talking about death or “giving up” more frequently
- Repeating the same stories as if forgetting previous conversations
When to Act
Don’t wait for crisis.
Early intervention:
- Prevents deep isolation
- Reduces long-term healthcare costs
- Improves recovery and quality of life
The earlier the action, the greater the impact.
Cultural Considerations in America’s Diverse Senior Population
Unique Challenges by Community
Hispanic/Latino Seniors
Strong family networks offset by language barriers in healthcare settings. Traditional multi-generational living arrangements provide built-in social connection, but immigration patterns sometimes separate families geographically.
African American Seniors
Church communities provide strong support networks, but historical healthcare mistrust complicates early intervention. Programs that partner with trusted faith communities show higher participation rates.
Asian American Seniors
Cultural stigma around mental health prevents help-seeking for loneliness. Many families view loneliness as a private matter not to be discussed outside the home, delaying critical interventions.
LGBTQ+ Seniors
Lifetime discrimination experiences create reluctance to access traditional senior services. Many LGBTQ+ elders lack family support systems and require specialized, welcoming programs.
Culturally Appropriate Solutions
Successful interventions acknowledge cultural values and communication styles. Faith-based programs show remarkable effectiveness across all cultural backgrounds when appropriately adapted to respect traditions and community norms.
Family Action Plan: Steps That Save Lives and Money
Immediate Assessment (Week 1)
Loneliness often hides behind silence. The fastest way to uncover it is to ask directly.
Start with simple, powerful questions:
- “When did you last have a meaningful conversation with someone?”
- “Do you feel lonely more than once a week?”
- “Are you avoiding activities you used to enjoy?”
These simple questions, similar to the validated UCLA 3-Item Loneliness Scale, can reveal hidden isolation. Don’t assume silence means contentment.
Create Support Structure (Month 1)
Build Regular Contact Schedule
Consistency matters more than duration.
- Daily or alternate-day calls
- Weekly in-person visits (if possible)
- Scheduled video calls with family
Even brief, predictable interactions can significantly reduce loneliness by creating a sense of stability and belonging.
Address Practical Barriers
Many seniors aren’t isolated by choice—but by logistics.
Address:
- Transportation challenges
- Hearing or vision issues
- Financial limitations
Fixing these often leads to immediate improvements in social engagement.
Connect with Community
Senior centers, faith communities, and volunteer opportunities provide purpose and connection. Local Area Agencies on Aging can identify resources in your parent’s community.
Long-term Monitoring (Ongoing)
Health Advocacy
Discuss loneliness with healthcare providers during visits. Request screening using standardized tools like the UCLA Loneliness Scale.
Resource Navigation
Connect with national programs like AARP Foundation’s Connect2Affect, which provides free assessments and personalized resource connections based on individual isolation risks.
Self-Care for Caregivers
Prevent family isolation while supporting seniors. Caregivers who become isolated themselves cannot effectively help others—build your own support network.
Professional Resources and Expert Insights
Healthcare Provider Training
Dr. Julianne Holt-Lunstad, Brigham Young University researcher, emphasizes: “Social relationships should be considered a public health priority, particularly for prevention.”
Medical Screening Tools
Progressive healthcare systems now incorporate:
- UCLA Loneliness Scale (3-question version): Takes under 2 minutes, with 77% sensitivity and 61% specificity for detecting loneliness.
- Social isolation assessment: Integrated during routine medical visits
- Electronic health records integration: Flags at-risk patients automatically
Community Partnership Models
Successful Programs Include:
- AARP Foundation Connect2Affect: National social isolation resources with personalized assessment tools
- Senior Planet: Technology and community engagement programs teaching digital skills in group settings
- National Association of Area Agencies on Aging: Local support networks connecting seniors to community resources
Frequently Asked Questions
1. What are the warning signs that an aging parent is lonely?
Look for increased medical complaints like headaches without clear causes, changes in sleeping or eating habits, and behavioral shifts like avoiding activities they once enjoyed. Frequent calls about minor concerns can also signal a need for connection. Pay attention to whether they linger at the end of phone calls or doctor visits, reluctant to end the conversation.
2. Is social isolation really as dangerous as smoking?
Yes. The U.S. Surgeon General reports that the impact of loneliness on life expectancy is similar to smoking 15 cigarettes a day. Isolation creates biological stress that significantly increases risks for heart disease, stroke, dementia, and early death.
3. How much does senior loneliness cost families financially?
Families often pay an additional $3,000 to $5,000 annually per isolated senior in out-of-pocket expenses. These costs stem from higher prescription needs, more emergency room visits, increased specialist consultations, and a doubled risk of entering nursing homes compared to socially connected seniors.
4. Can loneliness cause dementia or memory loss?
Loneliness significantly increases the risk of developing dementia, anxiety, and depression. While not a direct cause, isolation accelerates cellular aging and cognitive decline, often mimicking or worsening early symptoms of dementia. The inflammation and stress hormones caused by chronic loneliness damage brain tissue over time.
5. How do I know if my parent is lonely or just introverted?
Loneliness involves distress about social disconnection, whereas introversion is a preference for solitude. If your parent exhibits anxiety, physical symptoms like unexplained fatigue or pain, or expresses feelings of being a burden, they are likely experiencing loneliness rather than enjoying healthy solitude. Introverts recharge through alone time; lonely people suffer from it.
6. Does technology actually help reduce senior loneliness?
Yes, when paired with proper training and support. Simple tools like large-button phones and tablets with simplified video interfaces are effective. However, technology should supplement human connection, not replace meaningful face-to-face conversations. Studies show best results when older adults receive group training from peers close to their age.
Discover which senior health trackers offer life saving value and which ones are simply clever marketing. To know more about wearable tech options for senior safety, read our in-depth guide Wearable Health Tech for Seniors in 2025 – Hype vs Reality
7. What is the difference between loneliness and depression?
Loneliness is specifically the distress felt from a lack of social connection, while depression involves persistent sadness and loss of interest in activities. Though loneliness increases the risk of developing depression, they are distinct conditions requiring different support approaches. Loneliness improves with social connection; depression typically requires professional mental health treatment.
Find out if your forgetfulness is just a sign of a tired brain or a critical early warning for Alzheimer’s and Parkinson’s that you can still act on today. To learn more about early warning signs of cognitive decline, read our detailed guide Is Your Brain Getting Tired – Spot Early Signs & Prevent Alzheimer’s & Parkinson’s
Key Takeaways for American Families
Senior loneliness represents both crisis and opportunity. The crisis affects millions, costing billions in healthcare expenses while destroying quality of life. The opportunity lies in proven interventions that work when implemented systematically.
Action Steps
- Screen senior family members using direct questions about social connection
- Address practical barriers to social engagement like transportation and hearing
- Connect with community resources and healthcare providers who can help
- Monitor progress and adjust interventions based on results
Prevention Focus
Building social connections before crisis prevents both health deterioration and financial devastation. The economic evidence is clear: investing $1,500 annually in prevention programs saves $3,000-4,000 in healthcare costs per senior.
Stop worrying about dangerous falls and discover the breakthrough 2026 strategies that keep seniors steady, safe, and independent at home. Read our insightful guide Fall Prevention That Actually Works: Protecting Seniors in 2026
At higoodhealth.com, we’re committed to sharing evidence-based health information that empowers families to make informed decisions. We encourage you to explore our other resources on healthy aging, community health, and preventive care strategies from leading healthcare systems worldwide.
Share your experiences and suggest topics you’d like us to cover. Together, we can build healthier communities for all generations.
Glossary
Biomarkers: Biological indicators measured in blood or tissue that show disease or health status
C-reactive Protein (CRP): Blood marker indicating inflammation levels in the body
Cortisol: Primary stress hormone that affects multiple body systems when chronically elevated
Interleukin-6: Inflammatory protein that increases during stress and illness
Social Prescribing: Healthcare approach that refers patients to community programs for non-medical support.
Telomeres: Protective caps on chromosomes that shorten with age and stress
UCLA Loneliness Scale: Validated tool for measuring subjective feelings of loneliness and social isolation
Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult qualified healthcare professionals for diagnosis and treatment of medical conditions. Individual experiences may vary, and readers should verify information with their healthcare providers before making health-related decisions.
All reference links valid and accessible on 11 MaY 2026
AARP Public Policy Institute – Medicare Spends More on Socially Isolated Older Adults
U.S. Department of Health & Human Services – Surgeon General’s Advisory on Social Connection
University of California San Francisco – Dr. Carla Perissinotto Research
University of Michigan – National Poll on Healthy Aging: Loneliness Among Older Adults
Lines for Life – Senior Loneliness Line
AARP Foundation Connect2Affect
National Institutes of Health – Economic Costs of Loneliness and Social Isolation
UCLA Loneliness Scale (Version 3)
National Institute on Aging – Social Isolation and Loneliness Resources
Centers for Disease Control and Prevention – Loneliness and Social Isolation
World Health Organization – Social Isolation and Loneliness
Administration for Community Living – Connect with Area Agencies on Aging
Harvard Health Publishing- What is cognitive reserve?


