How Your Digestive System Shapes Your Mood, Mental Health, and Well-Being
TL;DR
- Your gut and brain are in constant two-way communication through the gut-brain axis, a network involving the vagus nerve, hormones, immune signals, and trillions of gut microbes.
- About 90% of serotonin is produced in your gut. Disruptions in gut health can contribute to anxiety, depression, brain fog, and mood disorders.
- Supporting your gut through diet, probiotics, stress management, and vagus nerve stimulation may improve both digestive and mental well-being.
- Gut-focused care complements but does not replace professional mental health treatment.
ntroduction: Why Your Gut Matters More Than You Think
Humans have always sensed a connection between the gut and the brain, whether it’s a “gut feeling,” a “gut-wrenching” experience, or a sudden stomach upset during moments of stress. But until recently, science had no clear explanation for this.
Now, emerging research is uncovering just how powerful this link truly is. Your digestive system doesn’t just break down food; it also plays a key role in how you feel, think, and respond emotionally.
Your gut houses its own neural network of over 100 million neurons, often called the “second brain” or the enteric nervous system (ENS). This system constantly exchanges signals with your brain and may influence your mood, stress responses, and emotional resilience. Understanding this communication pathway is transforming how researchers and clinicians view mental health.
What Is the Gut-Brain Axis, and Why Does It Matter?
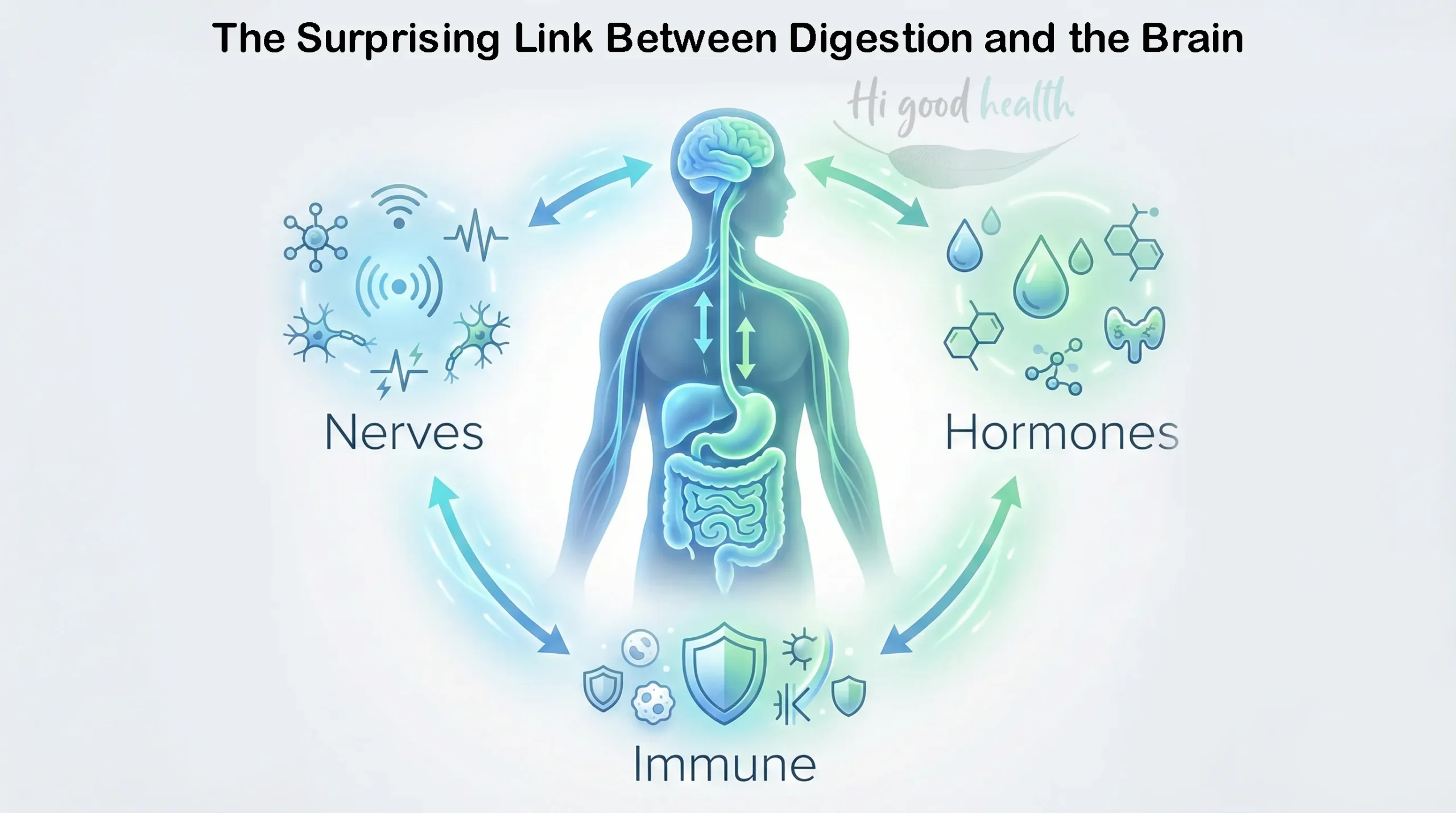
The gut-brain axis is a bidirectional communication system between the gastrointestinal (GI) tract and the central nervous system (CNS). It operates through multiple pathways:
- Neural pathways: The vagus nerve serves as the primary communication highway, carrying signals in both directions.
- Hormonal signals: Gut hormones and neuropeptides travel through the bloodstream to influence brain function.
- Immune signals: Cytokines and inflammatory markers produced in the gut can cross the blood-brain barrier and affect mood.
- Microbial metabolites: Short-chain fatty acids (SCFAs), neurotransmitter precursors, and other metabolites produced by gut bacteria act as chemical messengers.
When your gut is in balance, this system supports calmness, cognitive clarity, and emotional regulation. When it’s disrupted, it can contribute to anxiety, depression, brain fog, and memory issues.
Read more: Vagus Nerve as Modulator of the Brain–Gut Axis — Frontiers in Psychiatry
How Do Hormones and Immune Signals Influence the Gut-Brain Axis?
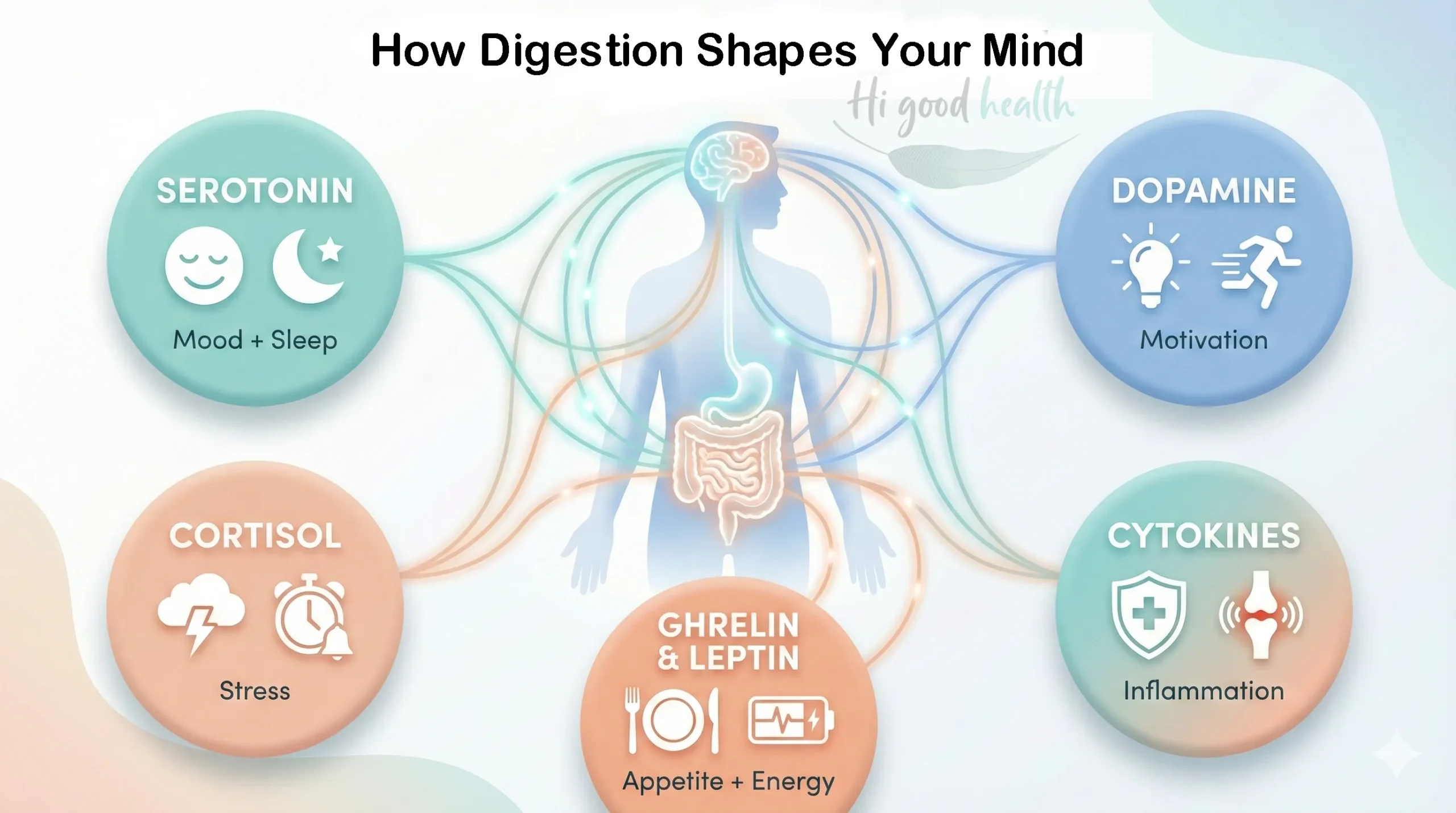
Several key chemical messengers help the gut and brain communicate. These include neurotransmitters, hormones, and immune molecules that affect your mood, stress levels, and mental health.
1. Serotonin
- About 90% of the body’s serotonin is produced in the gut by enterochromaffin cells, with gut bacteria playing a key regulatory role.
- Serotonin helps regulate mood, sleep, appetite, and digestion.
- An imbalance in gut-derived serotonin pathways is associated with anxiety and depressive symptoms.
2. Dopamine
- Approximately 50% of the body’s dopamine is produced in the gastrointestinal tract.
- Gut microbes help regulate dopamine pathways by producing precursor molecules.
- Dopamine affects motivation, pleasure, and reward. Low levels are linked to mood disorders.
3. GABA (Gamma-Aminobutyric Acid)
- Certain gut bacteria, including Lactobacillus and Bifidobacterium strains, can produce GABA.
- GABA is the brain’s primary inhibitory neurotransmitter, essential for reducing anxiety and promoting calm.
4. Cortisol
- Cortisol is the body’s primary stress hormone, released by the adrenal glands via the HPA (hypothalamic-pituitary-adrenal) axis.
- Chronic gut inflammation can activate the HPA axis, leading to elevated cortisol levels.
- Sustained high cortisol increases stress and anxiety, and can further damage the gut lining, creating a vicious cycle.
5. Cytokines (Immune Signals)
- These are proteins released during immune responses, particularly during gut inflammation.
- Elevated pro-inflammatory cytokines can cross the blood-brain barrier and interfere with neurotransmitter activity.
- Linked to brain fog, fatigue, and depressive symptoms.
6. Gut Peptides: Ghrelin & Leptin
- Ghrelin (“hunger hormone”) and leptin (“satiety hormone”) signal the brain about energy status.
- These peptides also influence emotional behavior, anxiety levels, and mood.
How Do Gut Microbes Communicate With the Brain?
Your gut contains trillions of microorganisms collectively known as the gut microbiota. These microbes do far more than aid digestion. They help produce neurotransmitters such as serotonin, dopamine, and GABA, which are chemicals that directly regulate mood and behavior.
When gut bacteria are diverse and balanced, they contribute to emotional resilience and a stable mood. But an imbalance known as dysbiosis can disrupt this harmony. Research has linked dysbiosis to increased stress reactivity, mood swings, and a lower threshold for anxiety.
Gut bacteria also produce short-chain fatty acids (SCFAs) like butyrate, propionate, and acetate through dietary fiber fermentation. SCFAs strengthen the intestinal barrier, reduce inflammation, and directly signal the brain via the vagus nerve and bloodstream.
Can Digestive Problems Affect Emotional Well-Being?
Many individuals with gastrointestinal disorders such as irritable bowel syndrome (IBS), acid reflux, or chronic constipation also experience mental health symptoms, including irritability, low energy, and persistent nervousness.
This isn’t purely psychological. Inflammation and discomfort in the gut send distress signals to the brain through the vagus nerve and immune pathways. These signals can activate the HPA axis, raising cortisol levels. Elevated cortisol, in turn, intensifies both digestive and mental symptoms.
According to Harvard Health Publishing, the brain and gut are so closely connected that digestive health can significantly impact emotional state and vice versa. Psychologically-based treatments like CBT and gut-directed hypnotherapy have shown meaningful improvements in both GI and mood symptoms.
- Gut disorders often coincide with mental fatigue, low motivation, and brain fog.
- Gut inflammation activates stress pathways in the brain.
- Elevated cortisol may worsen digestive discomfort.
- Recurrent gut issues can contribute to persistent anxiety or irritability.
- Treating gut symptoms may help reduce emotional strain.
What Role Does the Vagus Nerve Play in Mental Health?
The vagus nerve, also called the “wandering nerve” since it is the longest cranial nerve in the body, runs from the brainstem to the abdomen. It acts as the main communication highway between the brain and the gut, carrying approximately 80% of its signals from gut to brain (afferent) and 20% from brain to gut (efferent).
Stimulating the vagus nerve through deep breathing, meditation, cold exposure, or certain probiotics has been shown to improve mood, reduce inflammation, and decrease symptoms of depression. Researchers are also exploring vagus nerve stimulation (VNS) as a therapeutic intervention for treatment-resistant depression, with FDA-approved devices already in clinical use.
How Can You Support the Vagus Nerve and Restore Gut-Brain Balance?
Restoring balance in the gut-brain axis can improve both mood and digestive health. Here are evidence-supported lifestyle strategies:
- Practice deep, diaphragmatic breathing: Slow belly breathing (inhale 4 seconds, hold 4, exhale 6–8) activates the vagus nerve and lowers cortisol, or box breathing – 4-4-4-4 rhythm of inhale -> hold -> exhale -> hold
- Eat a gut-friendly diet: Probiotics, which include fermented foods like yogurt, kefir, kimchi, sauerkraut, and prebiotics such as oats, apples, and leeks, taken together maintain a balanced gut microbiome.
- Meditate regularly: Mindfulness meditation calms the nervous system and enhances vagal tone, the measure of vagus nerve activity.
- Exercise consistently: Moderate physical activity, such as walking, swimming, or yoga, supports both gut microbial diversity and mental well-being.
- Prioritize quality sleep: Sleep regulates mood, immune function, and the circadian rhythms of gut bacteria. Aim for 7–9 hours nightly.
- Stay socially connected: Positive social interactions have been shown to stimulate the vagus nerve and reduce depressive symptoms.
- Consider targeted probiotics: Certain strains like Lactobacillus rhamnosus and Bifidobacterium longum have shown mood-supporting effects in clinical studies. Always consult a healthcare provider before starting supplements.
Is There a Gut Connection When SSRIs Are Prescribed for Mood Disorders?
Yes. The gut plays a significant role even when someone requires medication like SSRIs (selective serotonin reuptake inhibitors) for serotonin-related mood disorders.
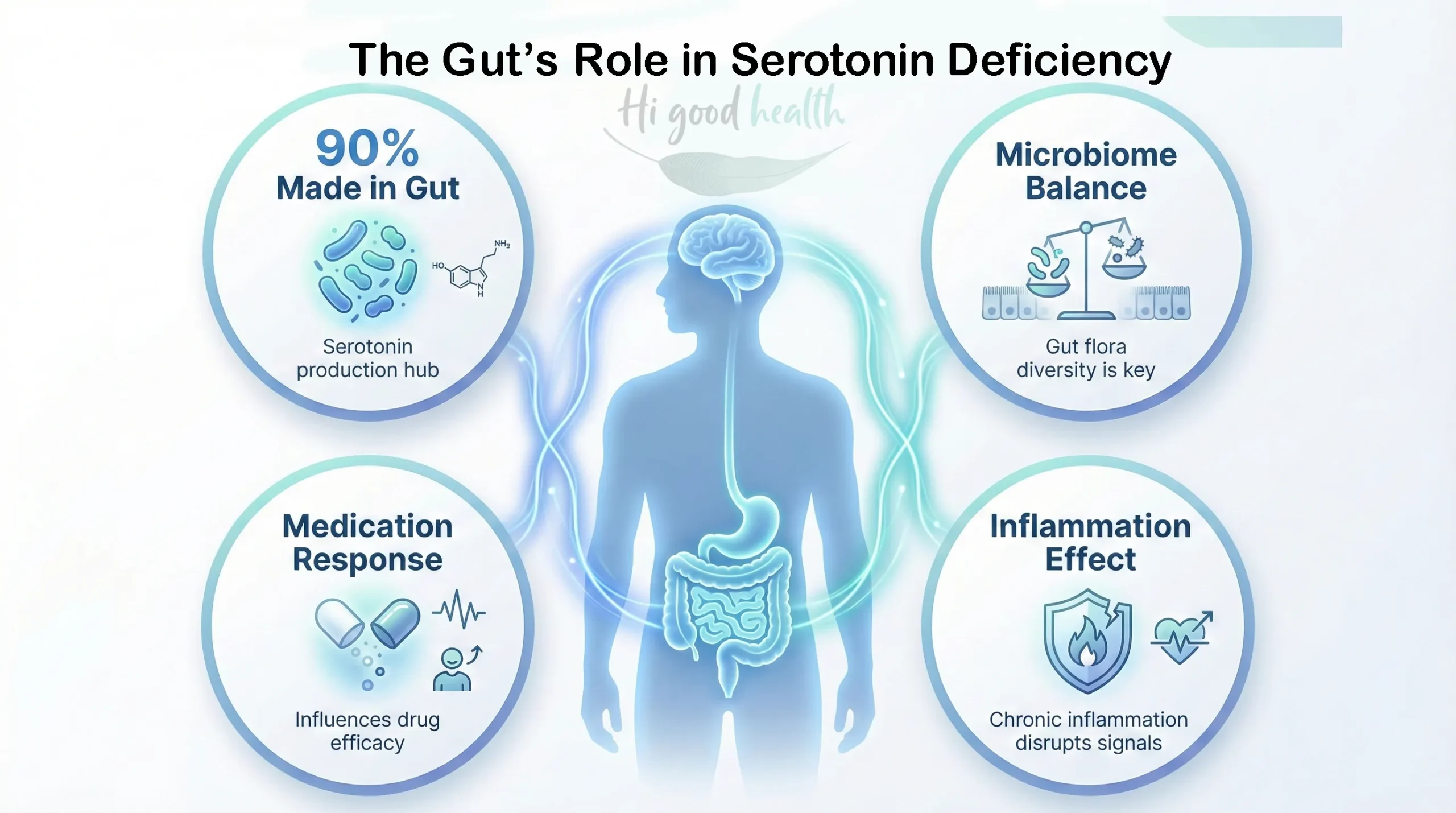
- Most serotonin is gut-derived: 90% of the serotonin is produced in the gut, even though it does not cross the blood-brain barrier, it influences mood by sending signals to the brain via the vagus nerve. Brain serotonin production relies on tryptophan, a tiny amino acid. When the gut is healthy, it ensures enough tryptophan is available to the brain.
- Gut bacteria regulate serotonin pathways: Certain microbes help produce or regulate serotonin. Dysbiosis can reduce serotonin availability and worsen mood symptoms.
- Medication effectiveness may depend on gut health: Emerging research suggests a healthy gut microbiome can enhance how well antidepressants work. Poor gut health might reduce effectiveness or increase side effects.
- Inflammation disrupts serotonin: Chronic gut inflammation directs tryptophan to be consumed by the Kynurenine pathway, instead of being sent to the brain to make serotonin – “the happy hormone.”
- Diet and probiotics as supportive measures: While medication remains essential for many patients, supporting gut health with a balanced diet, targeted probiotics, and anti-inflammatory foods may complement treatment outcomes. Never stop or adjust medication without medical guidance.
How Does Stress Impact Gut Health?
Stress triggers a cascade of chemical reactions in the body that affect gut function almost instantly. You may notice bloating, cramps, or an upset stomach during stressful periods. This is a documented biological response mediated by the HPA axis and the autonomic nervous system.
Chronic stress can:
- Reduce blood flow to the digestive tract, impairing nutrient absorption.
- Increase stomach acid production and irritate the intestinal lining.
- Shift gut bacteria composition, reducing beneficial species.
- Increase intestinal permeability (“leaky gut”), allowing harmful substances into the bloodstream.
- Trigger systemic inflammation, which further disrupts the gut-brain balance.
Over time, this cycle can contribute to both functional digestive disorders (like IBS) and mood disturbances. Addressing stress through evidence-based techniques is essential for long-term gut healing.
Can Probiotics Improve Mental Health?
Probiotics are live microorganisms that, when consumed in adequate amounts, confer a health benefit. Certain strains have shown promising effects in clinical trials for improving mood and reducing anxiety. These specialized probiotics are sometimes called “psychobiotics.”
- Some clinical trials suggest that Lactobacillus and Bifidobacterium strains may help reduce anxiety and depressive symptoms.
- Probiotics can reduce inflammatory markers such as C-reactive protein (CRP) in the gut.
- They may enhance serotonin and GABA production through microbial metabolic pathways.
- Results vary by strain, dose, and individual — not all probiotics have mental health benefits.
- Always consult a healthcare provider before starting psychobiotic supplements, especially if taking medication.
What Foods Support the Gut-Brain Connection?
Your gut thrives on fiber-rich and fermented foods. These feed beneficial bacteria, reduce inflammation, and support the production of mood-regulating chemicals.
| Food Category | Examples | Why It Helps |
| Fermented Foods | Yogurt, kefir, kimchi, sauerkraut, miso | Introduce beneficial bacteria and support microbial diversity |
| High-Fiber Foods | Oats, legumes, vegetables, fruits, and whole grains | Feed beneficial bacteria; produce SCFAs that reduce inflammation |
| Omega-3 Rich Foods | flaxseeds, walnuts | Support brain structure, reduce neuroinflammation, strengthen gut barrier |
| Polyphenol-Rich Foods | Berries, dark chocolate, green tea, olive oil | Act as prebiotics; have anti-inflammatory and antioxidant effects |
| Tryptophan-Rich Foods | cheese, nuts, seeds | Provide the precursor amino acid for serotonin production |
On the other hand, processed foods, artificial sweeteners, excess sugar, and ultra-processed snacks can harm your microbiome, promote inflammation, and negatively affect your mood. Hydration, regular meals, and mindful eating further support digestive and emotional balance.
Is There a Link Between Gut Inflammation and Depression?
Yes. Research increasingly supports that chronic, low-grade gut inflammation often leads to systemic inflammation, which is strongly associated with depressive symptoms. The mechanism involves:
- Inflammatory cytokines produced in the gut can alter brain function and reduce the production of mood-enhancing neurotransmitters.
- The kynurenine pathway, activated by inflammation, diverts tryptophan away from serotonin production toward neurotoxic metabolites.
- A poor diet, lack of sleep, and prolonged stress all contribute to this inflammatory cycle.
- Anti-inflammatory diets (such as the Mediterranean diet) and proper gut care are being studied as key strategies to restore mental balance.
Should Mental Health Treatment Include Gut Care?
The evidence increasingly supports integrating gut health into mental health care. Mental health treatment is evolving beyond the traditional brain-only model, with integrative approaches now focusing on the gut as a key player in emotional and cognitive health.
1. The Microbiome-Mood Connection
Studies have found that people with depression and anxiety often have distinct gut bacteria profiles compared to healthy individuals. Specific strains like Lactobacillus and Bifidobacterium have shown promise in reducing anxiety and depressive symptoms in clinical trials. These are sometimes called “psychobiotics.”
2. Gut Inflammation and Brain Health
Chronic low-grade gut inflammation can trigger the release of inflammatory cytokines that cross the blood-brain barrier and affect neurotransmitter activity. This inflammatory process is increasingly linked to conditions like major depressive disorder and bipolar disorder.
3. Nutritional Psychiatry
A growing field, nutritional psychiatry explores how diet affects mental health. Diets rich in fiber, polyphenols, omega-3 fatty acids, and fermented foods support a healthy gut environment and may boost the production of mood-regulating chemicals. The Mediterranean diet, for example, has been associated with a lower risk of depression in multiple clinical studies. One such study was the SMILES Trial, which was the first major study to demonstrate the impact of dietary changes on mood disorders.
4. Personalized Gut Testing
Emerging diagnostic tools such as 16S rRNA gene sequencing and whole-genome shotgun metagenomics allow researchers to analyze an individual’s gut microbiota with increasing precision. While these tools are primarily used in research settings today, they point toward a future of individualized treatment plans that combine conventional therapies with dietary changes, targeted probiotics, and supplements tailored to a patient’s gut profile.
5. Complementary Therapies
Practices like yoga, mindfulness, and deep-breathing exercises do more than reduce stress — they also stimulate the vagus nerve, enhancing gut-brain communication and helping regulate inflammation.
Important: Gut-focused care does not replace medications or therapy, especially for moderate to severe mental illness. But it offers a valuable, evidence-based complementary layer of support that can improve overall quality of life. For many patients, combining psychotherapy, medication, and gut health strategies creates a more holistic path to healing.
Why Should You Care About Your Gut-Brain Health?
Your gut and brain are in constant dialogue. What affects one often affects the other. Ignoring this relationship can delay healing, both mentally and physically. But nurturing your gut through nutritious food, stress management, quality sleep, and targeted probiotics can create a healthier, more balanced mind.
As research evolves, it is becoming clear that good mental health often starts with good gut health. Start paying attention to your digestive system; it may be the key to how you feel, think, and live.
If you prefer a more visual version, check out our YouTube video here:
Frequently Asked Questions (FAQs)
Your gut houses its own neural network (the enteric nervous system) with over 100 million neurons that constantly send signals to your brain. When your gut bacteria are balanced, this system supports calmness and emotional regulation. An imbalance can lead to mood swings, anxiety, and depressive symptoms.
Common signs include persistent irritability, low energy, brain fog, fatigue, nervousness, and feelings of depression that coincide with digestive issues like bloating, constipation, or cramping. If you experience both digestive and mood symptoms, the gut-brain connection may be a factor worth discussing with your doctor.
Stress activates the “fight or flight” response, which redirects blood away from the digestive tract, increases stomach acid, and can cause cramps or bloating. Chronic stress also raises cortisol, which can damage the gut lining and alter bacterial composition.
Some clinical trials suggest that specific probiotic strains, sometimes called “psychobiotics,” may help reduce anxiety symptoms. Strains like Lactobacillus rhamnosus and Bifidobacterium longum have shown promising results. However, not all probiotics have mental health benefits; strain, dose, and individual factors matter. Consult a healthcare provider before starting any supplement.
Yes. About 90% of the body’s serotonin, a neurotransmitter that regulates mood, sleep, and appetite, is produced by enterochromaffin cells in the gut. Gut bacteria play a key role in regulating this production. However, gut serotonin and brain serotonin serve different functions, and the relationship between them is still being studied.
Focus on fermented foods (yogurt, kefir, kimchi, sauerkraut), high-fiber foods (oats, legumes, vegetables), omega-3-rich foods (walnuts, flaxseeds), and polyphenol-rich foods (berries, green tea, dark chocolate). Minimize processed foods, excess sugar, and artificial sweeteners.
No. Gut-focused care is a complementary strategy and does not replace medication or professional therapy for mental health conditions. Supporting your gut may help medications work more effectively and reduce side effects, but never stop or adjust medication without consulting your prescribing doctor.
Deep, slow diaphragmatic breathing is one of the simplest and most effective methods. Try breathing in for 4 seconds, holding for 4 seconds, and exhaling for 6–8 seconds. Other techniques include cold water face immersion, humming or chanting, meditation, and moderate exercise.
High sugar intake and ultra-processed foods can harm the gut microbiome by promoting harmful bacteria and triggering inflammation. This gut inflammation is strongly associated with depressive symptoms and can interfere with neurotransmitter production. Reducing sugar intake and eating whole foods may help improve both gut health and mood.
Key Takeaways from Hi Good Health
The gut-brain connection is one of the most exciting frontiers in health science. The evidence is clear: what happens in your gut profoundly affects your brain, and vice versa.
Here’s how to start taking action today:
- Assess your diet — increase fiber, fermented foods, and omega-3s while reducing processed foods and sugar.
- Manage stress — practice daily deep breathing, meditation, or yoga.
- Talk to your doctor — discuss whether probiotics or gut-focused testing could complement your current health plan.
- Explore related content — check out our other articles on gut health, inflammation, and nutrition (links throughout this article).
All reference links valid and accessible on 20 March 2026
Medical Disclaimer: This article is for informational and educational purposes only and does not constitute medical advice. Always seek the guidance of a qualified healthcare professional with any questions regarding a medical condition, treatment, or medication. Do not disregard professional medical advice or delay seeking it because of information in this article.
